The Health Insurance Crash of 2025: What's Behind the Selloff, And How to Fix It
by Neil Ahuja, Founder / CEO
When "recession-proof" becomes free-fall, and billions vanish overnight
The Current Landscape: Rising Costs, Collapsing Confidence
The health insurance sector is in crisis. Once considered recession-proof, even the largest and most diversified health plans have seen their stock prices collapse in 2025. Medicare Advantage, Medicaid, and ACA exchange lines of business, long viewed as engines of growth, are now under pressure due to unanticipated spikes in utilization, regulatory scrutiny, and reimbursement misalignment.
Over the course of just a few months, tens of billions in market cap have been erased. Insurers are missing earnings, pulling guidance, and scrambling to explain cost overruns. Wall Street has responded swiftly and decisively. But this crisis is more than a momentary shock. It reflects a systemic failure in how payers monitor and manage real-time medical cost trends.
Top tip
The common thread across every earnings miss: health plans are flying blind on utilization trends until it's too late. By the time cost spikes show up in quarterly reports, the damage is already done.
The Carnage: Performance of Major Public Health Insurers (as of July 23, 2025)
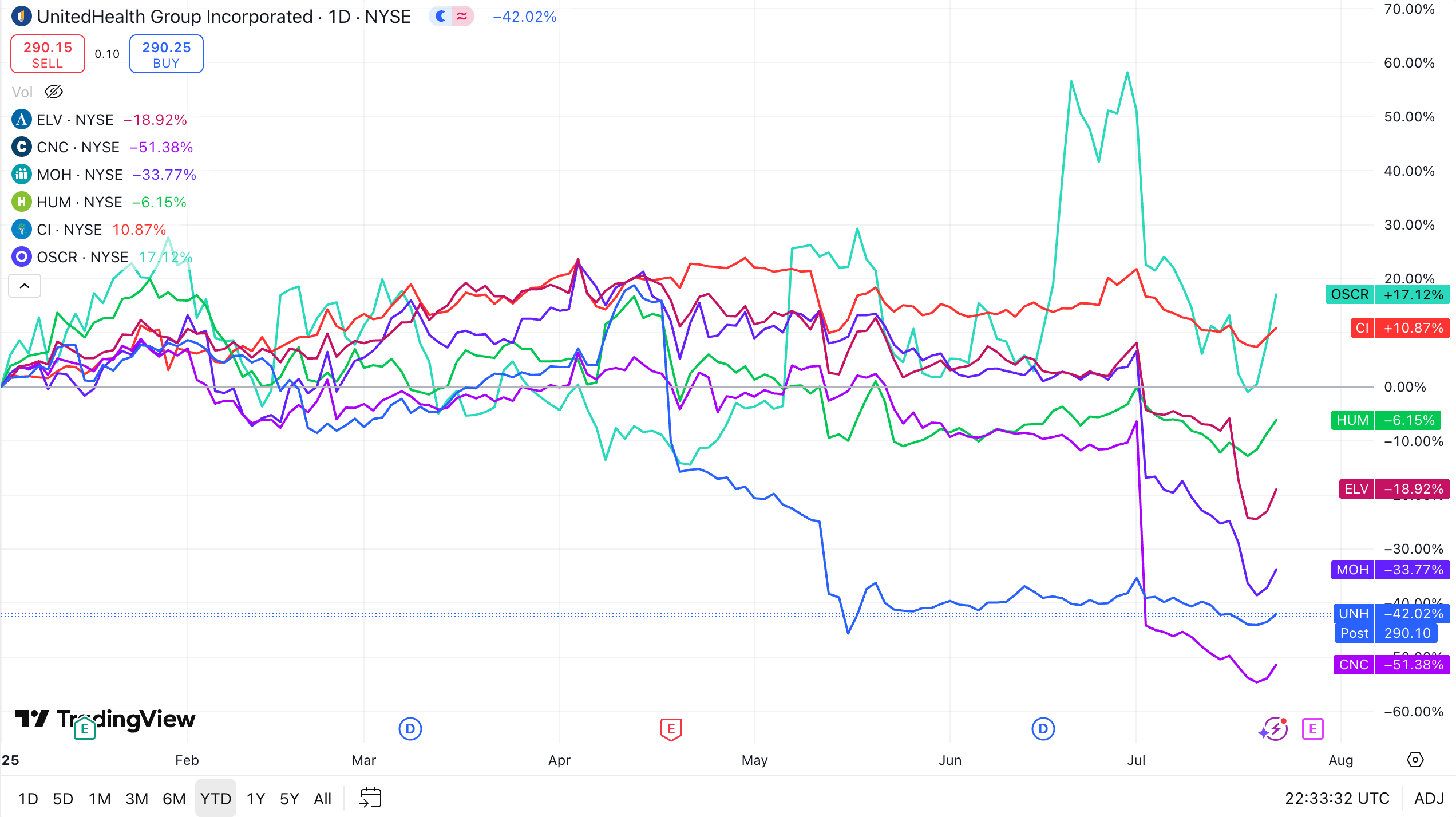
The numbers tell a devastating story:
| Company (Ticker) | YTD Return | 1-Year Return | Commentary – Why Stock Is Down |
|---|---|---|---|
| UnitedHealth (UNH) | −42.0% | −47.3% | Missed Q2 earnings for first time since 2008; rising Medicare Advantage costs drove medical loss ratio (MLR) to 84.8%. Pulled 2025 guidance, citing cost unpredictability. DOJ overbilling probe and sudden leadership shakeup added to investor uncertainty. |
| Elevance (ELV) | −18.9% | −41.0% | Earnings miss and full-year guidance cut due to elevated Medicaid and ACA utilization. Sector-wide sentiment turned negative after their warning. |
| Centene (CNC) | −51.4% | −54.7% | Pulled full-year guidance mid-Q2. Revealed ACA exchange enrollees were sicker than expected, suggesting EPS cut of up to 40%. Sparked broad ACA selloff. |
| Molina (MOH) | −33.8% | −33.7% | Cut earnings outlook due to rising ACA and Medicaid costs. Echoed concerns voiced by Centene and Elevance, triggering a similar decline. |
| Humana (HUM) | −6.2% | −38.6% | Continued MA cost pressures; while less vocal in earnings downgrades, stock is down in sympathy with peer turmoil and cost trends. |
| Cigna (CI) | +10.9% | −9.5% | Held up better than peers but still experiencing MLR pressure. Valuation compressed by broader selloff in health insurers despite stable fundamentals. |
| Oscar Health (OSCR) | +17.1% | +1.8% | ACA-heavy model flagged as vulnerable after Centene warning. Margins pressured by persistently high MLR. Downgraded by analysts due to limited pricing power and ongoing operating losses. |
Top tip
Even UnitedHealth, the industry giant, missed earnings for the first time since the 2008 financial crisis. When the "safe" stock drops nearly 50%, you know the entire sector is fundamentally broken.
The Solution: How Falcon Helps Health Plans Navigate the Storm
The common thread across these declines is a lack of real-time insight into rising utilization and risk. Falcon's AI-powered utilization monitoring tool is built to solve this. By analyzing claims and clinical data in near real-time, Falcon gives health plans early-warning signals about cost blowouts before they show up in quarterly financials.
Whether it's a sudden spike in ER visits among ACA members, dialysis utilization in Medicaid, or changes in inpatient coding patterns in MA, Falcon surfaces these signals instantly, allowing payers to take corrective action, reprice products, or trigger care management.
Top tip
In today's volatile market, the ability to anticipate cost drivers instead of reacting to them is the difference between leading the market and being punished by it.
The Revenue Recovery Play: Closing the Risk Adjustment Gap
In addition to real-time utilization monitoring, Falcon offers Scope, a next-generation risk adjustment reconciliation engine that helps Medicare Advantage and ACA plans recover millions in missed revenue. Scope ingests raw claims, encounter data, CMS files, and provider records, then uses AI to reconcile every diagnosis and treatment pair against medical guidelines and eligibility policies (LCD/NCD, InterQual, MCG). It also tracks the OIG audit methodologies and applies expanded OIG-style audits to identify potential issues before they become regulatory findings. The platform flags legitimate but undocumented or dropped risk-adjusted conditions and produces audit-ready evidence for submission.
Top tip
In a landscape where plans are bleeding margin from both under-coding and over-utilization, Scope delivers a powerful double benefit: it ensures compliant RAF capture while maintaining full CMS audit standards.
As plans face RADV clawbacks and volatile membership acuity, Scope ensures nothing is left on the table, legitimately and defensibly.
The Bottom Line: When health insurers are losing billions to utilization surprises and revenue leakage, the survivors will be those with the best early-warning systems and recovery tools in place.
The health insurance sector's worst crisis in decades demands more than hope. It demands better data, faster insights, and smarter tools. The question isn't whether you'll face these challenges, but whether you'll be ready for them.